
When we talk about restoring a tooth, we are not simply referring to “filling a hole.” Modern dentistry has come a long way: we restore anatomy, texture, and color so that no one can tell an intervention ever took place. It is a blend of health and art. If you have suffered a fracture, have deep decay, or bruxism has taken its toll on your teeth, dental reconstruction is the path to eating, speaking, and smiling with confidence again.
What does saving a tooth really involve?
Many people confuse a filling with a reconstruction. While the basic principle is similar — removing damaged tissue and replacing it — the scale and the goal are different. A filling treats small cavities, usually caused by early-stage decay. When the damage is extensive and affects one or more cusps of the tooth or the incisal edge, a more complex restorative architecture is required.
This is where the specialist’s expertise comes into play: restoring the structural integrity of the tooth. Imagine your tooth as a house that has lost a load-bearing wall; a simple patch is not enough — the structure must be rebuilt so it can support the “roof,” which in the mouth means the surprisingly intense forces of chewing.
Saving a tooth involves assessing how much healthy tissue remains, its position in the mouth, the occlusion (how the teeth fit together), and the patient’s habits. The goal is not just to make it look good, but to make it functional and long-lasting: able to withstand chewing pressure and integrate harmoniously with the rest of the mouth without causing joint or muscle problems.
Composite dental reconstruction
One of the stars of conservative dentistry is composite: a synthetic resin that bonds micromechanically to the tooth and can closely mimic natural enamel. Not all composites — and not all hands — perform the same, which is why technique and professional experience make such a difference.
Composite dental reconstruction is most commonly used when the damage is moderate. It is a direct treatment, usually completed in a single session. Its main advantage is tissue preservation: only diseased tissue is removed, while healthy structure is respected as much as possible.
The layering technique
To achieve an invisible result, the material is not placed all at once. Instead, a layering technique is used: layers of different opacities and shades. First, a layer that simulates dentin (the darker inner part of the tooth), followed by layers that replicate enamel (translucent and glossy).
This process requires time and precision. If you have seen fillings that look gray, opaque, or flat, the internal anatomy was likely not respected. With proper layering, the vitality of the tooth is restored by recreating grooves, mamelons, and unique characteristics that allow natural integration with the rest of the smile.
Advantages and limitations of composite
Advantages: preservation of tooth structure, direct repairability, relatively affordable cost, and immediate aesthetic results. Limitations: greater susceptibility to staining over time (coffee, tea, tobacco) and, in cases of extreme forces or large tissue loss, lower resistance than indirect ceramic restorations.
Dental veneers for broken teeth
In the so-called “social zone” of the smile, front teeth require a solution that is both aesthetic and durable. Trauma, a fall, or biting something hard can fracture an incisor. When the fracture mainly affects the visible surface of the tooth, veneers are often the ideal option.
The use of dental veneers for broken teeth offers superior aesthetics and good durability. Unlike a localized reconstruction, the veneer covers the front surface of the tooth, acting as both an aesthetic and functional shield.
Materials and selection
Veneers can be made from direct composite applied in the clinic, laboratory-fabricated composite veneers, or ceramic veneers (porcelain or lithium disilicate). Each material has its advantages: ceramics offer excellent color stability and high translucency; composite veneers are easier and more affordable to repair and require less tooth reduction.
The choice depends on the patient’s age, the extent of the fracture, habits such as bruxism, and aesthetic expectations. In younger patients or athletes, reversible and repairable solutions are often preferred; for definitive high-aesthetic restorations, high-quality ceramics are usually chosen.
Differences between a veneer and a simple reconstruction
If a tooth is broken at an unfavorable angle, a simple composite bonding may detach over time due to leverage when biting. A veneer provides a larger bonding surface and distributes forces more evenly. In addition, materials such as porcelain maintain color and shine for years, while composite may yellow or lose gloss over time.
Alternatives for severe damage: Inlays and Crowns
When the remaining structure is insufficient, direct filling can be counterproductive: the tooth may fracture vertically down to the root and ultimately require extraction. To prevent this, indirect restorative dentistry is used.
Inlays and Onlays
These are the intermediate option between a large filling and a crown. If much of the chewing surface has been lost but healthy walls remain, an impression is taken — now almost always with a 3D digital scanner — and a ceramic or hardened resin piece is fabricated in the laboratory. It fits like a puzzle and restores function without excessive tooth reduction.
Full-coverage crowns
These are reserved for severely compromised teeth, often after root canal treatment. The crown fully encases the tooth, protecting it from fracture and restoring shape and occlusion. Modern ceramic crowns provide excellent aesthetic results and good strength.
In teeth with wall loss and a risk of root fracture, it may sometimes be necessary to place an intraradicular post before fabricating the crown, reinforcing the structure and ensuring reliable adhesion.
Dental reconstruction Before and After
A broken tooth that does not contact its opposing tooth can lead to headaches, neck tension, or temporomandibular joint problems. Reconstruction aims to restore balance to the entire chewing system: shape, function, and aesthetics.
Below, we show a recent case of incisal edge fracture repair carried out in our clinic.
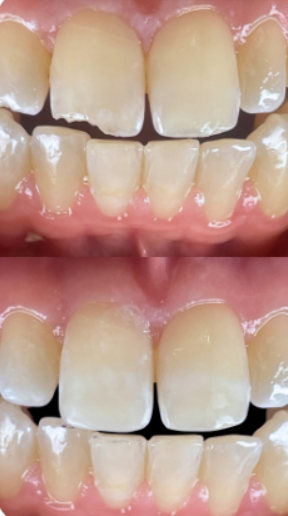
Does the procedure hurt?
The short answer: it shouldn’t. Modern dentistry prioritizes patient comfort. For deep reconstructions, local anesthesia is applied to completely numb the area; you may feel pressure or vibration, but not sharp pain.
In teeth that have already undergone root canal treatment, anesthesia is sometimes not necessary, although many professionals still administer it for comfort and to reduce patient stress, especially when the session is long or involves multiple techniques.
After the procedure, mild sensitivity may appear for a few days, particularly with extreme temperatures. This usually subsides with mild analgesics and proper oral hygiene. If sensitivity persists or worsens, it is advisable to return to the professional for a check-up.
At Centro Dental Smiling, we know that every tooth matters and that a well-executed reconstruction can last for decades when performed with the right protocols and care. Do not let a broken tooth stop you from smiling — in many cases, the solution is simpler and less invasive than you might imagine.




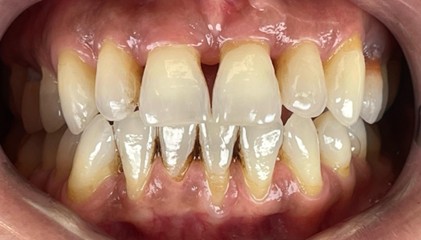










 Periodontal Surgery
Periodontal Surgery


 Preventing dental curettage at home
Preventing dental curettage at home