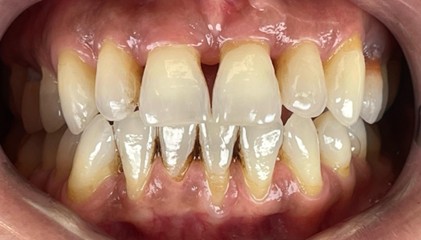
Looking in the mirror and noticing that your teeth seem “longer” than usual, that small dark spaces have appeared between them, or that your gums no longer look as healthy as before can be deeply unsettling. It affects not only your oral health, but also the appearance of your smile and your confidence.
Advanced periodontitis, commonly known as pyorrhea, is a disease that affects the supporting structures of the teeth. Beyond the clinical explanation, we know it has a direct impact on self-esteem. So, can aesthetic treatments such as veneers be used in patients with periodontitis? The short answer is yes — but with very important considerations.
Understanding the relationship between gums and smile aesthetics
Before talking about aesthetic materials or techniques, we need to talk about the foundation.
Advanced periodontitis causes progressive bone loss around the teeth. As the bone recedes, the gum tissue follows, exposing the root of the tooth, which is narrower and more yellow than enamel. This process also creates the well-known black triangular spaces between teeth.
These spaces are not just an aesthetic concern. They easily trap food and bacteria, making oral hygiene more difficult and increasing the risk of further periodontal problems.
Any aesthetic solution must therefore be designed not only to close gaps, but also to allow proper cleaning and maintain tooth stability. Ignoring the balance between function and aesthetics often leads to medium-term failure.
Initial assessment: what do we evaluate during the first visit?
During the first consultation, we assess tooth mobility, periodontal pocket depth, bone loss on radiographs, and the level of inflammation control. We also analyse smile type, gum exposure, and enamel quality. All of this determines whether periodontal treatment must come first or if aesthetic rehabilitation can already be planned.
Using composite restorations in periodontitis patients
When discussing veneers for patients with periodontitis, composite restorations are often preferred over ceramic or porcelain options, although every case is unique. Why is composite frequently the material of choice in these situations?
The main reason is its conservative nature and versatility. Teeth affected by periodontal disease have reduced bone support. Aggressive preparation for crowns or porcelain veneers may weaken them further. Composite allows for an additive approach: instead of removing tooth structure, material is added to restore lost form.
Composite also makes it possible to splint teeth together. This means that slightly mobile teeth can be joined both functionally and visually, improving overall stability. In addition, if gum levels change over time — which is possible in periodontal patients — composite restorations can be repaired directly in the clinic, unlike porcelain, which often requires full replacement.
When composite is recommended — and when it is not
Composite is ideal for patients looking for a conservative, repairable solution with minimal tooth preparation. However, in cases involving severe bruxism or areas where long-term optical stability and translucency are critical, ceramic may be considered — provided tooth structure allows it and mobility is well controlled.
The Bioclear Method
One of the most advanced aesthetic solutions for patients with advanced periodontitis is the Bioclear Method. This technique has transformed the way we manage the aesthetic consequences of periodontal disease.
Traditionally, closing black triangles with conventional fillings was difficult and often resulted in over-contoured margins that irritated the gums or stained over time.
The Bioclear technique uses special transparent matrices placed around the tooth, allowing for an ideal anatomical shape below the gum line. Heated composite is injected into these matrices, creating a smooth, monolithic and highly polished restoration. By fully wrapping the tooth, the black triangle is closed while also supporting the papilla, helping it maintain its position.
This approach is minimally invasive. No healthy tooth structure needs to be removed. Instead, the tooth is “dressed” to restore its original volume and close the spaces created by bone and gum loss. For many patients, it offers a natural-looking solution without compromising dental integrity.
Advantages and limitations of the Bioclear Method
The main advantages include maximum preservation of tooth structure, fast treatment times, and easy repairability. Limitations include the need for precise technique and excellent polishing to prevent plaque accumulation. Long-term success depends heavily on periodontal stability and proper maintenance.
Periodontal treatment: before and after aesthetics
This is the cornerstone of any successful treatment. Under no circumstances should veneers or aesthetic restorations be placed on inflamed, bleeding gums. The first step is always to stabilise the periodontal disease.
This usually involves a thorough hygiene phase, including deep scaling and root planing to remove subgingival calculus and reduce bacterial load.
Periodontal treatment before the aesthetic phase is what separates long-term success from failure. The goal is to eliminate infection and allow the gums to reattach firmly — even if this initially makes the teeth appear longer. Although visually challenging for patients, this phase is essential.
Once the periodontist confirms that the disease is inactive (even if it remains a chronic condition requiring lifelong monitoring), aesthetic rehabilitation can begin. This is where cosmetic dentistry helps correct the visual consequences left by periodontal disease.
Before:
After:
The importance of oral hygiene in advanced periodontitis solutions
No aesthetic treatment, regardless of its quality or cost, will succeed without excellent oral hygiene at home. Any solution for advanced periodontitis must be supported by a strict daily routine.
The use of interdental brushes is essential. When gaps are closed with composite or veneers, the anatomy between teeth changes, and patients must learn how to clean these new contours properly. We provide personalised guidance to ensure effective cleaning without damaging restorations.
Brushing techniques, specific toothpaste recommendations, and — when appropriate — antiseptic gels or mouth rinses are also reviewed. Professional maintenance visits every 3 to 6 months are crucial to detect any signs of recurrence early.
If you recognise these symptoms or are unsure whether you are a suitable candidate for aesthetic treatment after periodontitis, an individual assessment is essential. Every mouth is different, and the extent of bone loss will determine which techniques and materials are safest in the long term.
Professional registration Nº 28004040
Degree in Medicine and Surgery, Autonomous University of Madrid
Degree in Dentistry, Complutense University of Madrid
Master’s Degree in Aesthetic Dentistry, Complutense University of Madrid
University Specialist in Pediatric Dentistry, San Rafael Hospital, Madrid
University Specialist in Individual and Public Oral Preventive Programs, Complutense University of Madrid
Director of Radiodiagnostic Facilities
Medical Director, Smiling Dental Center
Specialist in Aesthetic Dentistry, Dr. Bruce Crispin, Los Angeles, California
Member of the Spanish Society of Prosthodontics (SEPES)
CPR Course
Advanced English